
The Dementia Hospital Stay
A hospital stay can be challenging for anyone, but for individuals with dementia, it can be particularly daunting. The unfamiliar surroundings and the presence of strangers can lead to increased confusion and fear. In this article, we’ll explore what a hospital stay entails for someone with dementia and provide insights into how caregivers can navigate this experience.
Hospital Admission for People with Dementia: Unraveling the Reasons
People with Dementia may find themselves in the hospital for various reasons. Understanding the cause of admission is crucial, as it impacts the length and complexity of the hospital stay. Here are some of the most common reasons for hospital stays.
Increased Confusion:
One common reason for hospitalization is a notable increase in confusion experienced by individuals with Dementia. This heightened state of confusion might signal an underlying issue or a change in the person’s health condition. Recognizing and addressing the root cause of this confusion is crucial to providing appropriate care during the hospital stay.
Fainting and Falls:
Individuals with Dementia often face challenges in maintaining balance and coordination. This can lead to incidents of fainting or falls, resulting in injuries. Hospitalization may be necessary to assess and treat injuries and investigate the underlying factors contributing to these incidents. Understanding the circumstances surrounding falls is vital for devising preventive strategies.
Trauma and Injuries:
Trauma or injuries can prompt a hospital visit, whether accidental or resulting from other medical conditions. People with Dementia may be more vulnerable to accidents or injuries due to their cognitive limitations. Identifying the specific nature of the trauma and its impact on the individual’s health is crucial for devising a suitable treatment plan.
Heart Disease:
Individuals with Dementia are not immune to other health conditions, and heart disease is one such example. The complexity of managing both Dementia and heart-related issues requires specialized care. Hospitalization becomes necessary for a comprehensive evaluation of heart health and the implementation of appropriate interventions.
Stomach Issues:
Digestive problems, ranging from mild discomfort to more severe stomach issues, can prompt hospital admission for individuals with Dementia. Identifying the nature and severity of these stomach issues is essential for providing targeted and effective medical care. This includes considerations for the individual’s dietary needs and overall well-being.
🧭 “Preparation doesn’t remove all risks—but it reduces fear.”

Why Understanding the Cause Matters: Impact on Hospital Stay
The reason for hospital admission significantly influences how long a person with Dementia stays in the hospital.
Suppose the admission reason is a medical condition for someone who also has Dementia. Dementia may complicate the treatment plan and prolong the hospitalization because they are unable to follow directions or they become more confused. It is very common for a hospital stay with a common medical condition to be extended for someone with Dementia.
However, they are also at a higher risk for complications during their stay.
If the reason for the hospital visit is increased confusion, the hospital will usually keep them overnight to assess the reason for the change.
Sometimes, the primary caregiver decides they just can’t be a 24-hour caregiver anymore. They believe it is time for placement in an extended care facility, and a hospital stay can be the stepping stone needed to initiate placement.

Hospital Interaction with Dementia Patients: A Complex Challenge
Are you wondering if hospital staff care for your loved one the same way you care for them at home? Here are a few challenges to consider when deciding whether to leave your loved one in the hospital alone.
Not Enough Training:
Hospital workers, such as nurses and other healthcare staff, don’t always get enough training on how to help those with Dementia. Alzheimer’s and Dementia are difficult to understand and require special knowledge.
Many healthcare workers do not understand there are different types of Dementia with varying behaviors. Their understanding of how to interact with someone with Dementia to prevent escalating behaviors is also limited, which can complicate the care being provided.
Always in a Hurry:
Hospitals operate in a fast-paced environment, and staff members often have demanding schedules. The need to attend to multiple patients, handle administrative tasks, and respond to emergencies can result in a rushed approach to caregiving. Unfortunately, this hurried pace may inadvertently lead to increased frustration and agitation in dementia patients who require more time and patience.
Being Alone in the Hospital: Why it’s Hard for People with Dementia

What happens if you do leave a dementia person alone in the hospital?
Hospitals are Confusing:
Hospitals have many different things going on – strange noises, people walking around in uniforms, and complicated hallways. For someone with Dementia who needs a routine and familiar faces, it can feel really confusing and scary.
Call Buttons are Tricky:
Most hospitals rely on call buttons when a patient needs help. But for someone with dementia, that little button can feel like a complicated puzzle. They may not remember how to use it—or even understand what it does. So if they’re scared, in pain, or need the bathroom, they may have no way to alert anyone.
Simple Things are Tough:
Things we don’t think twice about—ordering a meal, finding the bathroom, answering a phone, or changing the TV channel—can become overwhelming challenges. Without help, they’re left feeling scared, embarrassed, and completely vulnerable. And that stress often shows up as agitation, confusion, or even behaviors that look like “acting out.”
🏥 “Hospitals treat illness; families protect the person.”
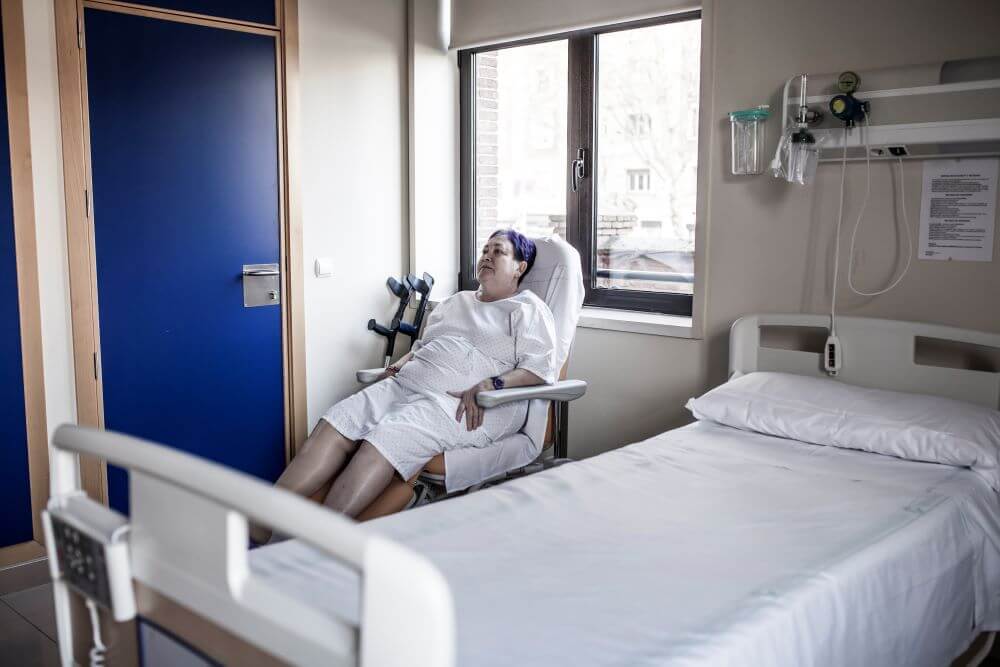
Challenges During the Stay: Navigating a Different Routine
We know keeping someone with Dementia in a routine is the best way to keep them calm and happy, but what happens to their routine in the hospital?
Unfamiliar Faces and Procedures:
Hospitals are filled with unfamiliar faces, including healthcare professionals and other patients. The constant presence of new people can be overwhelming for someone with Dementia, who relies on recognizing familiar individuals for comfort. Additionally, unfamiliar medical procedures and equipment can add to their anxiety and confusion.
Altered Schedules:
Daily routines often change in the hospital. Medication and meal times may not match what the person with Dementia is used to at home. This shift can be confusing, as they rely on familiar routines to feel secure. The changes may affect their overall well-being and contribute to feelings of disorientation.
Meal Times:
Hospital care for patients usually revolves around the hospital’s schedule. Therefore, the medication and meal times are different than at home. Most hospitals switched from scheduled routine trays to self-ordering whenever the patient was hungry.
That works well for the alert and oriented patient, but what about someone with Dementia? Your loved one depends on the staff to order their tray and help them eat if family is not there to help. Unfortunately, trays often get ordered late, and when they arrive, they may sit at the desk and get cold.
Keep in mind that there may be ten patients on the unit who all need to be fed, and only three nursing staff members can help. It also may take a while to feed someone with Dementia. Most people in the later stages of Dementia are very slow eaters, and it may take 30-60 minutes to feed one person.
Sleep Disruptions:
Hospitals have different schedules for checking vital signs and other medical procedures, which can interrupt sleep. For someone with Dementia, being woken up from their sleep can be disorienting and lead to increased confusion. Sleep disruptions often contribute to behavioral challenges and may impact the overall mood and well-being of the patient.
Sleep time in the hospital is interrupted every couple of hours for vital signs or toileting. For many Dementia patients, once they settle down and get to sleep, someone they don’t know wakes them up in the middle of the night.
Once they are woken up, they are more confused than usual. A strange person, strange place, and no one they recognize often leads to agitation/aggressive behavior. The hospital staff’s response to this aggressive behavior is usually a behavior medication. This medication has a sedating effect and can last well into the next day, which may result in them sleeping through their meals and more confusion.

The After-effect of a Dementia Hospital Stay
Many family members are surprised to find their loved one has drastically declined after a hospital stay. Recognize that this is a real possibility. A Dementia hospital stay can lead to a decline in several areas.
Increased Confusion:
A stay in the hospital can often lead to heightened confusion for individuals with Dementia. The change in environment, unfamiliar faces, and the hustle and bustle of the hospital setting can contribute to disorientation. This increased confusion is especially noticeable post-hospitalization and may persist for some time as the person adjusts back to their home or care facility.
Exacerbation of Cognitive Decline:
For individuals with Dementia, any disruptions to their routine or environment can exacerbate cognitive decline. The stress of a hospital stay, coupled with the impact of medical procedures and medications, may accelerate the progression of dementia symptoms.
Changes from Anesthesia and Medication Adjustments:
The very nature of a hospital stay involves significant changes. Anesthesia, often used for various procedures, can have lingering effects on cognition and increase confusion. For some people with Dementia, anesthesia seems to push them into the next stage of the disease, where they may stay. However, after a while, others bounce back to where they were before the hospitalization.
Additionally, adjustments or changes in their routine medications during the hospitalization process can impact cognitive function, potentially leading to a decline in mental clarity.
Decreased Mobility:
Lying in a hospital bed for an extended period can quickly lead to weakness — especially in older adults. Muscle loss can begin in as little as 24–48 hours of bed rest.
Even just 2–3 days in bed can make it difficult for them to get up on their own.
It’s not uncommon for someone who was walking independently at home before hospitalization to suddenly need one or even two people to help them get out of bed. What feels like “just a few days” can turn into a major setback in strength and independence.
That decline can happen fast.
This is why it’s so important to encourage your loved one to sit up in a chair for all meals and walk to the toilet whenever possible. Keeping them moving helps protect their strength, balance, and confidence.
If you’re concerned about weakness, don’t be afraid to ask the doctor or nurse about a physical therapy evaluation while they’re still in the hospital. Early movement and therapy can make a big difference in how well they recover.
Bladder Changes, Catheters, and Mobility Decline
People with dementia often struggle with bladder incontinence as the disease progresses. They may feel urgency, have accidents before they can get to the toilet, or lose the ability to recognize the need to void.
At home, caregivers usually learn the signs. Many even use a scheduled toileting routine to prevent accidents and protect dignity.
But in the hospital, things change.
Your loved one may need help pressing the call button or waiting for staff to assist them to the bathroom. Staff may not be able to respond right away. This can lead to more frequent incontinence. Over time, some patients begin urinating while lying in bed because it becomes easier than waiting.
Unfortunately, that pattern can continue after discharge.
Your loved one may also have a urinary catheter (internal or external) placed during their hospital stay. While catheters are sometimes medically necessary, they come with risks.
Many families don’t realize:
-
Catheters significantly increase the risk of urinary tract infections (UTIs).
-
UTIs can cause sudden confusion, agitation, falls, and even hospitalization again.
-
Staying wet or soiled increases the risk of skin breakdown and pressure injuries.
-
The less someone gets up to use the toilet, the weaker they become.
The bladder is a muscle. When a catheter does all the work, the bladder can become “lazy.” Some patients truly struggle to restart normal voiding once the catheter is removed.
And here’s something most people don’t think about…
For many elderly individuals, walking to the bathroom several times a day is their primary form of exercise. It keeps their leg muscles active. It maintains balance. It preserves independence.
When toileting stops, movement stops.
When movement stops, weakness begins.
Maintaining a toileting routine — even in the hospital — is imperative to preserving mobility.
If a catheter is suggested, it’s okay to ask:
-
Is this medically necessary?
-
How long will it stay in?
-
Can we remove it as soon as possible?
Protecting mobility often starts with protecting the simple act of walking to the bathroom.
Dementia Hospital Stay Beds
The length of stay in a hospital varies for those with Dementia, especially if there are complications. However, they must be discharged from the hospital once they are medically stable. Many families struggle with the decision to release the patient and try to keep their loved ones in the hospital longer.
The COVID-19 pandemic stressed all hospitals and created many complicated patients who still go in and out of the hospital.
As a result, hospital beds are in high demand, and the demand shows no signs of letting up.
Hospitals are now caring for sicker and more severe patients than ever before. Extended care facilities have become step-down units.
Medical issues that used to require a week in the hospital are now only requiring a two—to three-day stay. Many patients are sent to a facility to continue physical therapy, IV antibiotics, or other medical treatment.
Discharge Planning for a Dementia Hospital Stay
Discharge planning starts early in the hospitalization process, often long before families feel ready. The hospital team—usually a discharge planner or case manager—will look at your loved one’s home care needs, their safety, and the level of support they will need once they leave the hospital.
What surprises many families is how quickly this conversation happens. You may barely be settled into the room before the discharge planner appears, asking about the home environment, available caregivers, and who will be helping once your loved one is discharged. For dementia caregivers, this can feel overwhelming and rushed—especially if the hospitalization was unexpected.
This is why it helps to understand the process ahead of time and be prepared to talk through the discharge plan. The hospital must ensure your loved one will be safe once they leave, and they will expect you to participate in making those decisions. Having some idea of your options can make this transition smoother and far less stressful.
Caregivers should communicate early with the discharge specialist so they can explore realistic options, including the possibility of short-term rehab or extended care facilities.
Extended care facilities are often discussed for individuals in the middle to late stages of dementia, especially when the family is overwhelmed, there are signs of caregiver burnout, or the hospitalization has caused a sudden decline. This is the point where families often hear for the first time that their loved one may not be safe returning home without more support.
Discover the Key to Understanding Alzheimer's & Dementia
💡 Dementia can feel overwhelming, but when you understand what’s happening, patience becomes easier.
The Understanding-Dementia Course gives you the tools to prepare, cope, and care with more peace.


Why You Should Explore Facilities Before You Need Them
Many caregivers wait until a crisis forces their hand—after a fall, a hospitalization, or a sudden change in condition. At that point, decisions are made quickly, under pressure, and with limited time to research.
Looking into facilities ahead of time can make an enormous difference. It gives you the chance to:
-
Learn what options exist in your area
-
Find facilities that understand dementia care
-
Ask questions when you’re calm—not in crisis
-
Compare waitlists, costs, and availability
-
Know which places accept your insurance
-
Have a “Plan B” ready if hospitalization causes a decline
-
Avoid last-minute decisions that feel rushed or overwhelming
Having a short list of places you trust doesn’t mean you’re “giving up.” It simply means you’re prepared—just like having a first-aid kit ready at home. Planning ahead protects both you and your loved one.
If you’re unsure whether you’re even close to needing this step, I encourage you to read How to Know When It’s Time to Get Help for Alzheimer’s or Dementia Care. That article walks you through the signs that more support may be needed—before a crisis makes the decision for you.
Hospital discharge planners can also offer options you may not know even exist, including respite stays, rehab programs, and memory care communities with short-term beds. But the more you know before you walk into the hospital, the easier these decisions will be.
If your loved one is in the hospital for more than 2–3 days, the discharge team may recommend a rehab facility. This is usually due to the need for physical therapy, strengthening, IV antibiotics, or additional medical care that can’t safely be done at home.
It is very common for people with dementia to require short-term rehab after hospitalization.
The key is not waiting until this moment to start learning about your options.
Knowing what’s available ahead of time gives you confidence, reduces your stress, and helps you speak up for what your loved one truly needs.
What to Look for in a Dementia-Friendly Facility
When researching facilities in your area, look beyond appearance and marketing brochures. Dementia-friendly care focuses on safety, consistency, and understanding—not just amenities.
Here are a few key things to look for:
-
Experience with dementia care (ask how staff are trained and how often)
-
Consistent staffing so residents see familiar faces
-
Calm, structured routines rather than rigid schedules
-
Clear communication with families about changes, behaviors, and health concerns
-
Secure environment to prevent wandering
-
Personalized care plans that consider routines, preferences, and triggers
-
Respectful behavior management that prioritizes comfort over sedation
-
Support for transitions, such as short-term rehab or respite stays
Taking time to ask these questions before a crisis gives you more control and confidence if you ever need to make a quick decision.
Know Your Local Options: Dementia Care Planning Checklist
You don’t need to make a decision today—but you do need to be informed.
This checklist helps family dementia caregivers understand what options exist before a hospital stay or emergency forces fast choices.
💡 “Knowledge turns panic into purpose.”

What is Hospital-Induced Delirium?
Delirium is scary! It comes on quickly and can become a medical emergency. Unfortunately, many hospitalized Dementia patients develop Delirium. According to John Hopkins, 80% of ICU patients and 1/3 of all hospital patients develop Delirium. Very sick patients and older adults who are hospitalized are especially at risk. “Developing delirium is linked to worse outcomes in older people in the hospital, and it is associated with a higher risk of declining health and death.”
Various factors can lead to Delirium. The most common include surgery, infection, isolation, dehydration, poor nutrition, and medications.
Delirium can last for an hour or days; some people never return to their previous state. It is prevalent in elderly hospitalized people, especially those with Dementia. It is a daily occurrence in most hospitals.
Treatment for Delirium consists of trying to identify the cause. Unfortunately, people who develop Delirium often become very aggressive and are given behavior medications to keep them from harming themselves or others. Generally, this medication can add to their confusion.
The signs of Delirium are:
Drowsiness
Confusion (new came on quickly)
Feeling disoriented
Hallucinations (seeing or hearing things not there)
Delusions (having false or unrealistic beliefs or opinions)
Delirium is not limited to hospital patients but can also happen at home. If you suspect delirium, notify your healthcare provider immediately
How Family Can Help While in the Hospital
Family involvement is one of the most important protections a person with dementia has during a hospital stay. You are the constant when staff changes, shifts rotate, and routines disappear.
Being prepared makes a real difference. Having key information ready helps prevent confusion, reduces stress, and allows staff to care for your loved one as a person—not just a patient.
Before heading to the hospital, gather important details in one place so they are easy to share when needed.
This information should include:
-
The name your loved one prefers to be called
-
Who holds medical power of attorney
-
Foods and drinks they enjoy (and dislike)
-
Their normal daily routine
-
Medication schedule and sensitivities
-
Bathing preferences and timing
-
Communication tips (what works and what doesn’t)
-
Activity level and mobility needs
-
Toileting routine
-
Typical sleep pattern
-
Favorite topics or memories to reminisce about
-
Religious or cultural preferences
-
What helps calm them when they are anxious or agitated
-
Common behaviors staff should be aware of
Keeping this information written down prevents repeated explanations and helps staff quickly understand how to approach and support your loved one.
ALZlog: The Caregiver’s Notebook is designed to organize all of this essential care information in one easy-to-use place—at home or in the hospital.
To make this even easier, you can download the free Getting to Know Me: Dementia Care Guide for Hospital Staff form and give it directly to nurses and providers. It offers a quick snapshot of who your loved one is, how they communicate, and what helps them feel safe.
A simple form. A powerful tool. And one less thing for you to worry about during a stressful hospital stay.
🌱 “Temporary confusion doesn’t mean permanent decline.”

Stay With Them if Possible
You or another family member should stay with them if at all possible. Many caregivers consider hospitalization a break from caregiving and stay home to get some much-needed rest. However, you are still needed. Nurses and doctors will need you to help answer questions and to be the patient liaison for your loved one.
So, if possible, pack a bag and set up camp in that room. Be there to recognize if Delirium is coming on and alert the staff to the changes. Here are a few tips to help both of you during a hospitalization.
- Ask for a recliner so you have a comfortable place to sleep
- Help the person fill out menu requests
- Remove personal clothes from sight
- Listen to soothing music or try comforting rituals, such as reading, praying, singing, or reminiscing
- Bring in familiar objects, such as photographs of family members or a pet
- Build a relationship with the nursing staff
Do not assume that the staff understands the realities of caring for someone with Dementia.
Instead, help them to understand your loved one and their needs. Try to avoid taking your loved one to the hospital if possible, for both your sakes.
Know your loved one’s wishes. Learn the difference between aggressive care and comfort care and what they desire as the disease progresses. If you or a loved one is in the early stages of the disease, please take a look at completing the Dementia Advanced Directives.
It is imperative to know what type of medical care is wanted as Dementia worsens.
❓ Questions Caregivers Often Ask
1. Is it normal for dementia symptoms to get worse in the hospital?
Yes. Hospitals are unfamiliar, noisy, and disruptive. Temporary confusion or delirium is very common—even with planned procedures.
2. What increases the risk of delirium during a hospital stay?
Pain, anesthesia, new medications, dehydration, infection, lack of sleep, and being moved between units all raise the risk.
3. How long does hospital-related confusion usually last?
It can be hours, days, or even weeks. Some people bounce back quickly. Others take longer—and some never fully return to their previous baseline.
4. What is the caregiver’s most important role in the hospital?
Advocacy. You know your loved one best. Staff may rotate, but you are the constant.
5. Can preparation really make a difference?
Absolutely. Simple steps—clear communication, written information, and early intervention—can prevent serious setbacks.
The Role of Caregivers: Patient Advocates for Loved Ones with Dementia
When your loved one is in the hospital, they need you to be more than just their caregiver. They need you to become their patient liaison.
Effective Communication:
Patient liaisons play a pivotal role as advocates for their loved ones with Dementia. Communicating the patient’s unique needs, preferences, and routines to the hospital staff is essential. This information empowers healthcare professionals to provide more personalized and considerate care. Sharing details about what calms the patient, their communication style, and any specific triggers helps create a more supportive environment.
Providing Insight:
They possess invaluable insights into the behavioral patterns and idiosyncrasies of the person with Dementia. This knowledge enables hospital staff to tailor their approach, minimizing potential sources of distress. Whether it’s a certain soothing gesture, a preferred way of communication, or activities that bring comfort, these insights guide healthcare professionals in delivering more patient-centered care.
Collaboration with Staff:
Establishing an open line of communication between caregivers and hospital staff fosters collaboration. Patient Liaisons can share information during admission, engage in regular updates with the care team, and participate in care planning discussions.
This collaborative approach ensures that the hospital staff is better equipped to meet the unique needs of the dementia patient.
In summary, acknowledging the challenges faced by hospital staff in dementia care and actively engaging with healthcare professionals as a caregiver and a Patient Liaison can significantly enhance the overall well-being of your loved one during their hospital stay.
Effective communication becomes the bridge between the medical team’s expertise and caregivers’ intimate knowledge of their loved ones.
💜 Final Thoughts
A hospital stay is never easy. And when Alzheimer’s or dementia is part of the picture, it can feel overwhelming, unpredictable, and even frightening.
But here’s what I want you to remember:
You are not powerless.
Preparation changes everything.
Understanding what might happen helps you stay calm when it does.
Knowing the risks allows you to prevent some of them.
When you understand how dementia affects the brain, you begin to see hospital behaviors differently. You recognize delirium sooner. You understand why routines matter. You know why mobility must be protected. You feel more confident speaking up.
And confidence lowers fear.
Every small step you take — from bringing a familiar photo to keeping a written care summary — protects your loved one. Every question you ask helps prevent unnecessary decline. Every time you stay present, you become their anchor in an unfamiliar world.
Hospital stays may be unavoidable.
But panic is not.
The more knowledge you have, the more peace you carry into the room.
💡 Knowledge turns crisis into clarity.
🌿 Want to Feel More Prepared Before the Next Hospital Stay?
Dementia doesn’t just affect memory — it affects judgment, behavior, communication, sleep, mobility, and reactions to stress.
When you understand what’s happening in the brain, you stop feeling blindsided.
You recognize:
✔️ Why hospital stays increase confusion
✔️ Why routines matter so much
✔️ Why behaviors escalate in unfamiliar places
✔️ What changes are likely coming next
🌿 Knowledge brings calm. Preparation brings confidence.
The Understanding Dementia Course walks you step-by-step through the stages of the disease, what to expect, and how to respond with clarity instead of fear.
You don’t have to keep guessing.
You can feel prepared.
Hi, I’m Larea, a Registered Nurse, Faith Community Nurse, and Certified in Dementia Care with 30 years of experience supporting families living with Alzheimer’s and other dementias. Both of my parents have Dementia, so I understand the journey personally as well as professionally. My heart is in helping family caregivers feel supported, prepared, and confident every step of the way.












Great article! Wonderful information and definitely will put ideas to use. Thank you!