Dehydration in Dementia: A Hidden Danger
As a caregiver, you likely settle into a routine with your loved one, which often brings some sense of calm. But in dementia care, change can come quickly, sometimes overnight. You might wake up to a completely different person than you saw the day before. Yesterday’s calm, mild-mannered loved one might now be angry, confused, and even throwing things.
If you’re an experienced caregiver, you might immediately think, “Uh-oh, this looks like a UTI!” But did you know dehydration in people with dementia can cause symptoms just like a urinary tract infection (UTI)? It’s one of those sneaky things that can really throw a wrench into your day.
What to Watch For: Signs of Dehydration
Spotting dehydration early is key because it can cause so many issues, from confusion to serious health problems. Knowing what to look for can help you catch it before it becomes severe. Some signs to be aware of are:
- Dry eyes, lips, and mouth – If they lick their lips often or if you notice cracks, dehydration might be to blame.
- Fatigue or weakness – Do they seem extra sleepy or struggle to move as usual?
- Decreased urination – If they’re going fewer than four times a day or haven’t gone in over eight hours, dehydration could be the culprit.
- Dark urine – It should be light, like straw. Darker shades signal dehydration.
- Dizziness or lightheadedness – Have they been complaining of feeling dizzy or unsteady on their feet?
- Confusion or agitation – Increased confusion or sudden behavior changes are big red flags.
- Muscle cramping – Especially in the arms or legs, cramps are common with dehydration.
- Development of UTIs – If UTIs keep cropping up, dehydration could be behind it.
Severe Dehydration: Time to Act Fast
When dehydration becomes severe, you need to act quickly. Some of the more serious signs include:
- Sunken eyes – Their eyes may look hollow or more recessed than usual.
- Decreased sweating – If you notice they aren’t sweating as they normally would, especially in warm weather, it’s time to be concerned.
- Trouble walking or fainting – They might be more unsteady or even collapse.
- Seizures – This is an emergency situation that needs immediate attention.

Why Does Dehydration Happen?
Dehydration happens to all older adults, not just those with dementia. Our bodies simply don’t hold water the way they used to. On top of that, underlying health issues like kidney disease or diabetes can cause the body to lose even more fluids. Medications are another common cause of dehydration. The main ones to watch out for are:
- Laxatives – These can flush too much water out of the body.
- Diabetic medications – Some affect the kidneys, making them pull more water out of the system.
- Diuretics – Often used to treat high blood pressure, these work on the kidneys to help the body urinate more, which can dry them out.
For people with dementia, the risk is even higher. They might forget to drink or not recognize when they’re thirsty. Eventually, they can’t communicate their needs, making dehydration a constant concern.
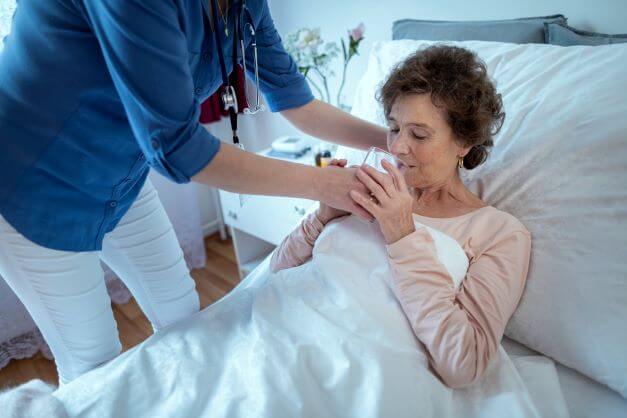
Tips to Prevent Dehydration
As a caregiver, you’ve probably had to get creative to keep them hydrated. Here are a few ideas that might help:
- Keep drinks within reach – Make sure water or their favorite drinks are always nearby.
- Use attractive cups – Sometimes a fun, colorful cup with a lid can be more inviting.
- Set reminders – If they’re in the earlier stages of dementia, setting an alarm or leaving notes to remind them to drink can help.
- Sweeten the deal – People with dementia often retain a sweet tooth, so offer them juices or flavored drinks. Popsicles can be a great way to get fluids in too—they’re fun and tasty!
- Fruits and veggies – Water-rich foods like watermelon, cucumbers, and oranges are great alternatives if they resist drinking.
- Mix it up – Offer a variety of drinks, from sports drinks to water, and even consider special hydration treats like Jelly Drops, which are made for people with dementia.

Remember, coffee and tea can have a drying effect, but if they love them, offer other beverages alongside to balance things out. Aim for 4 to 6 cups of fluid a day.
Dehydration and Delirium: A Dangerous Duo
Delirium is different from dementia but can make caregiving even harder. Delirium comes on suddenly—within a day or two—and can cause confusion, agitation, or dramatic personality changes. Dehydration is a big trigger for delirium, and once it sets in, it can take weeks or even months for your loved one to recover, if they ever do.
I’ve seen families have to make the heartbreaking decision to move their loved ones into nursing homes after a severe bout of delirium. The effects can be long-lasting, so it’s important to act fast if you notice these sudden changes.
Anyone can get Delirium, but those with Dementia are at a much higher risk.
Delirium can also be caused by:
- pain
- infection
- poor nutrition
- constipation or urinary retention
- dehydration
- low levels of blood oxygen
- a change in medication
- abnormal metabolism (for example, low salt or blood sugar levels)
- an unfamiliar or disorientating environment
Remember, the treatment for Delirium is to address the cause. If they are dehydrated, getting fluids in their system is the first line of treatment. Learn more about common dementia complications HERE.
End-stage Dementia and Dehydration
In the final stages of dementia, your loved one will lose their appetite and refuse food and drinks. Swallowing becomes difficult, and they may choke on what they do try to eat or drink. This is a natural part of the disease, and while it’s incredibly tough to watch, it’s a normal part of the body’s slow shutdown process. Learn more about the dementia stages HERE.
Many caregivers and families wonder if giving fluids via IV or tube is the right choice during this time. It’s important to know that dehydration at the end of life can actually reduce discomfort. Fluids given at this stage can build up in the lungs and cause more harm than good. This is a hard conversation to have, but talking about it early on can help you honor your loved one’s wishes and let nature take its course peacefully.

Conclusion
Dehydration in dementia can be a serious and often overlooked issue, but with a little extra care and attention, it’s possible to prevent it from happening or catch it early. Keeping your loved one hydrated is an ongoing challenge, but by being aware of the signs and offering a variety of drinks and water-rich foods, you can help them stay healthy and avoid complications like delirium or UTIs. Remember, every small effort to keep your loved one hydrated can make a big difference in their comfort and well-being. And as dementia progresses, it’s essential to have those important end-of-life conversations, so everyone is prepared to honor their wishes when the time comes.
Hi, I’m Larea, a Registered Nurse, Faith Community Nurse, and Certified in Dementia Care with 30 years of experience supporting families living with Alzheimer’s and other dementias. Both of my parents have Dementia, so I understand the journey personally as well as professionally. My heart is in helping family caregivers feel supported, prepared, and confident every step of the way.









0 Comments